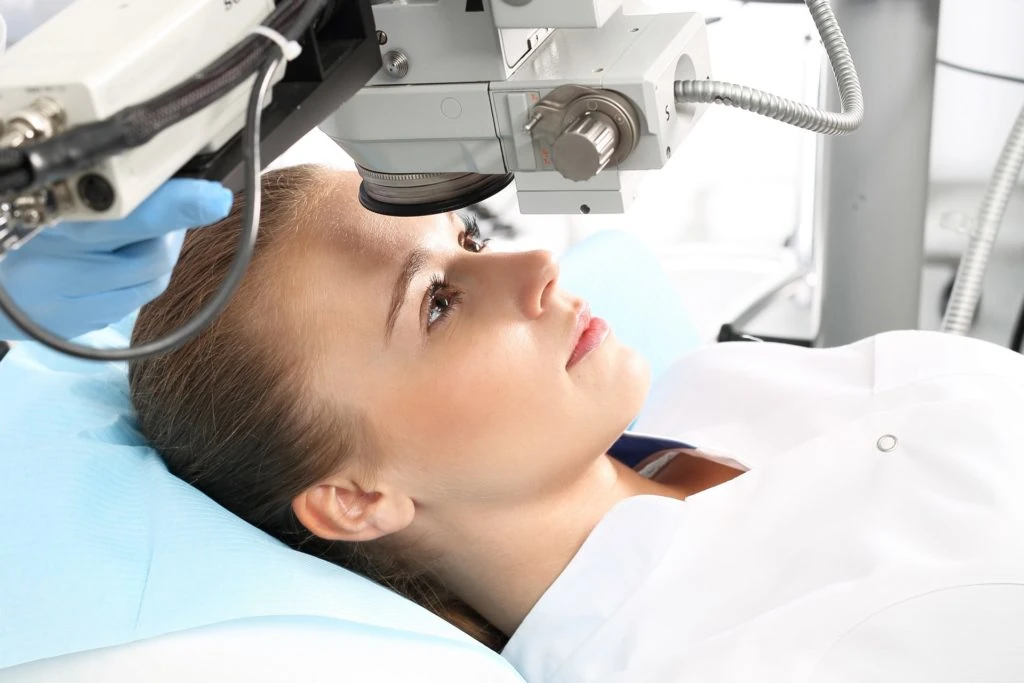
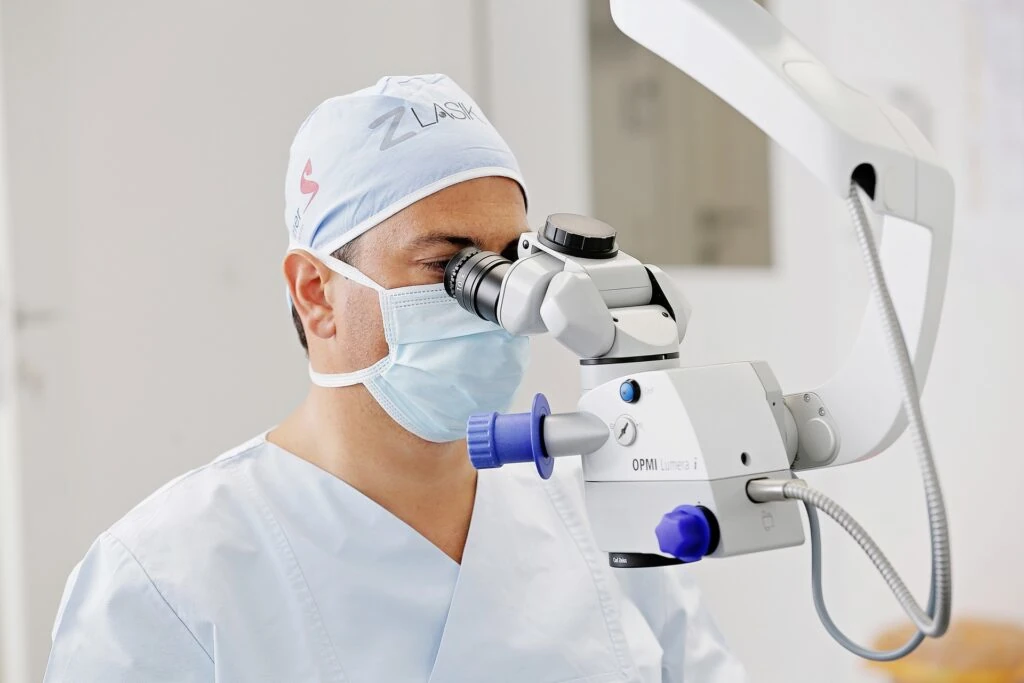
Management after cross linking procedure
Immediately after the procedure, the eye is painful and hypersensitive to light. The doctor recommends antibiotics and steroid drops. As part of the dressing and protection, the patient wears soft contact lenses for several days. Until the epithelial healing process is complete, various side effects, such as burning and watery eyes, may occur during the first two months. After successful eye treatment, the patient can return to hard contact lenses. As a rule, with CLX of the cornea of the eye, the desired goal of stabilization is achieved after the first treatment.
Corneal cross-linking of the eye is usually a very safe method that does not cause any serious side effects. Compared to corneal transplantation, it is also much cheaper. No serious complications associated with corneal crosslinking, such as damage to the retina or lens of the eye, have been observed to date. The complication rate of the procedure is less than 3%. None of the cases previously treated with corneal crosslinking also had a subsequent need for a corneal transplant. 98-99% of eyes previously treated with CLX achieved the desired corneal stabilization.
Experience has shown that many patients with keratotorus (PMD) can receive optical supplies with implantable contact lenses for permanent ametropia correction after about 6 months of UV cross-linking. In patients with corneal cone, due to the greater irregularity of the corneal curvature, contact lenses with stable dimensions or alternatively corneal ring segments (ICRS) are more suitable for optical treatment.
Can you stop wearing glasses after cross-linking surgery
After the crosslinking procedure, astigmatism is often much more regular than before. In this way, PMD patients in particular achieve good visual acuity under spectacle correction. There is also a chance to permanently correct vision by implanting implantable contact lenses made of biocompatible collagen (EVO VISIAN ICL).
Implantation should occur no sooner than 6 months after cross-linking, as the cornea may still change during this time. A combination of transepithelial crosslinking and ICL has already succeeded in freeing some patients from glasses and contact lenses.